A different kind of gold rush has come to Colorado.
Urine drug tests, long considered a relatively inexpensive and unremarkable medical procedure, cost the state of Colorado’s Medicaid program more than $1 million every month last year alone, according to an investigation by 9Wants to Know.
To put that into perspective, in late 2014, the same program spent a little more than $50,000 per month or urine tests.
INTERACTIVE: Colorado Medicaid spending on urine drug tests
Drug labs defend the expenditures as critical in fighting the ongoing painkiller addiction epidemic. Critics, however, call the burgeoning industry a profit grab.
“There’s just no other way to explain the numbers when it comes to urine drug testing,” said California attorney Harry Nelson, a nationally recognized expert on the subject who has written articles on the value of urine screens for years.
For more than two years, the cost to Colorado’s Medicaid program went largely unchecked. Only when 9Wants to Know discovered the data, did leadership within the program announce plans to review the sheer volume of tests being ordered.
Already, a member of Colorado’s legislature is calling our investigation “deeply disturbing.”
“This is the first I’ve heard about it,” said Rep. Joann Ginal (D-Fort Collins).
She’s hardly alone in that.
So in order to better understand what’s taking place here, let’s walk you back to the moment our investigation began.
It all started with an email to showusyourbills@9news.com
Chapter 1
$6,250 to pee in a cup
Sherryn Hensley’s email to 9Wants to Know on March 13 suggested the possibility of a story in its opening paragraph.
“Thank you for highlighting the ridiculous cost of health care. As a heart patient I am used to insane medical bills, however this one took the cake,” she wrote.


Later that day, she emailed me a copy of her “Explanation of Benefits (EOB)” from Cigna. While not a bill, it suggested she owed $6,250 to a company called Insight Labs for a round of urine tests.
Oddly enough, around that same time, I received a copy of another woman’s EOB also from Cigna. That EOB, from 2015, suggested the woman – who has chosen to stay anonymous – was charged $6,842 by a Texas-based lab for a round of urine screens.
Her EOB told her Cigna would cover $3,658.74, leaving her with $1,969.96 left to pay.
“I feel these bills are extreme,” the woman told me.
I quickly started calling urine screeners in order to find out how much a typical urine screen might cost.
Richard Matteucci, owner of USA Mobile Drug Testing, even agreed to come to 9News in order to help walk me through it.


“I can do a pretty good test for less than $100,” he said
How many drugs can you test?
Close to 20, he told me.
What if we wanted to test for more?
“It might run in the high $200s most likely,” he said.
His test wouldn’t tell me specifically how much of a drug was in the urine, he said, but it would find the presence of close to 20 drugs.
And there, I would later learn, lies the rub.
Chapter 2
Two different tests, two very different costs
In order to understand the world of urine screening and lab costs, you have to understand what brought Sherry Hensley into Dimensions Pain Management back in February.
Multiple surgeries have left Hensley with chronic pain near her heart.
“I’ve had 15 stents placed in the last 4 years,” she said.


At the time she went into the Louisville office, she was well aware of the potential problems associated with prescription painkiller addiction.
So she didn’t wince when the staff asked her to take a urine test.
Urine tests for pain management are now common, if not standard. In 2011, the National Institutes of Health released a study that showed, in part, “Compliance monitoring has been shown to be crucial in delivering proper opioid therapy and preserving this therapy for the future. Urine drug testing (UDT) is considered one of the mainstays of adherence monitoring in conjunction with prescription monitoring programs and other screening tools.”
In other words, those who needed pain pills needed to be ok with their pain management doctors testing their urine.
Hensley didn’t know it at the time, but her initial urine screen was the standard “pee in a cup” variety. Think of Matteucci’s $100 pee test.
Paperwork Hensley agreed to share with 9Wants to Know showed the original POC (Point-of-Care) test showed only the presence of barbiturates in her urine.
That was to be expected, however, as her paperwork shows the doctor who conducted the test had already noted a prescription for a Butalbital – a well-known barbiturate.
In every other drug category of the initial POC test, she tested negative, according to her medical records.
That didn’t stop the doctor from asking for an expanded round of testing.
Hensley’s medical records show Dr. Leif Sorensen proceeded to order a unique test for every category available on the Insight Labs order form.

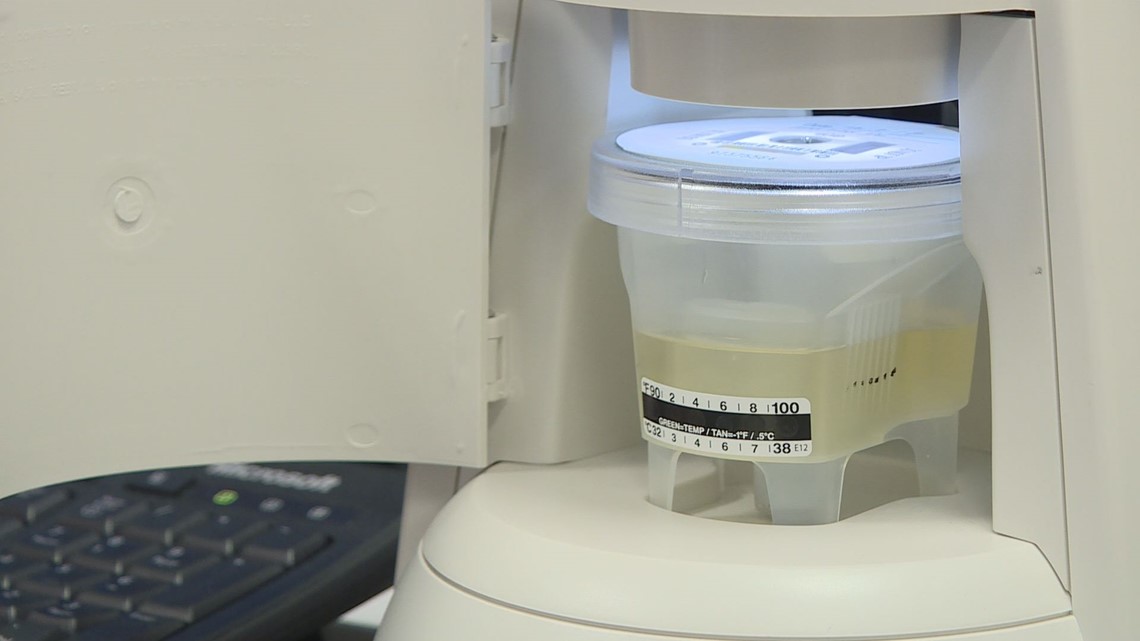
He wanted to know just how much of everything, from the street drugs ecstasy and meth to legal drugs such as oxycodone and tramadol, was in her urine. Keep in mind, she had already preliminarily tested negative for all of that.
We wanted to know why Dr. Sorenson ordered such large panel of tests for a patient with no history of drug abuse, but our calls to his office went unreturned.
Instead, the owner of his practice, Centura Health, responded with a written statement saying, in part, “We will not comment on the care provided to an individual patient.”
Regardless, once Insight Labs repeatedly tested her urine, one test after another, everyone learned what the original test had already concluded.
Her urine showed nothing unexpected. No cocaine. No ketamine. Nothing.
SHOW US YOUR BILLS: Fill out the form HERE
In all, her test results highlighted the word “negative” next to more than 50 drugs – some legal, some not.
Hensley’s EOB does not break down how many tests Insight billed her insurance, but the $6,250 charge indicates the lab billed Cigna for multiple tests. Medicaid, for example, will only reimburse around $16 per test in Colorado.
Other bills we’ve examined suggest it’s not unusual to charge more than a $100 for each test.
Regardless, Hensley’s insurance offered one more hiccup.
Her policy disallows coverage for any out-of-network charges, and Insight Labs is considered out-of-network with Cigna, according to Hensley.
It’s why Hensley’s EOB indicated she might owe the total amount charged.
Of course, there was at least one more wrinkle to sort through, however.
Chapter 3
Someone always pays
Recently, and after repeated denials of our interview requests, 9Wants to Know paid an unannounced visit to Golden-based Insight Labs with Hensley in order to understand more about the $6,250 charge.
There a nice lab technician told us we needed to contact the director of the lab, Justin Simons.
“We have already,” I replied. “He’s not calling me back.”
I then said Hensley, according to her insurance company, was still on the hook for the $6,250 charge.
That’s when he told us, on camera, “More than likely we’ll just be losing money on it.”
It was an answer that seemed to mesh with Insight’s own brochure that said, “Insight Laboratories… does not take actions that will negatively affect the patient or guarantor’s credit history.”
The lab doesn’t seem particularly interested in collecting money from people who can’t afford to pay.
A few days later, a spokesperson for the lab emailed me a statement telling me Hensley wouldn’t have to pay a dime. “As far as the cost to the patient – there is none. The services the patient received at the Insight lab will not be billed to them. Insight does not pursue collections in cases where the insurance is denying coverage.”
Colorado law specifically prohibits health care providers from waiving deductibles or copayments as a matter of “regular business practice.”


Attorney Harry Nelson said companies like Insight run the risk of violating the law when they simply forgive patient’s bills as a matter of routine business practice. Laws, like the one in Colorado, try to make patients have, in essence, some skin in the game in order to prevent them from always going with the more costly option.
Any hint that a patient’s bill will be forgiven might run counter to that.
“It’s telegraphing to the patient that [the bill] ‘is not going to be your problem. We’ll take what we can get from the insurance company and move on.’ That’s what insurance companies consider fraud,” he said.
Heather Wilson, a spokesperson for Insight, told 9Wants to Know in an email that Colorado’s law “applies to Medicare. This was not a Medicare situation.”
When informed that Colorado’s law also applies to private insurance, Wilson told us, “I talked to a lawyer – [Insight] is in compliance with the law.”
She wouldn’t elaborate.
So why the big hullabaloo if no one is going to have pay Hensley’s bill? As we found, what happened to Hensley is happening over and over again, and sometimes someone does pick up the tab.
Like you and me, for example.
Chapter 4
'Very concerning'
It appears private insurance companies are well on their way toward fighting back against possible misuse in the system.
When we informed Cigna that it paid more than $3,800 of a 2015 bill we reviewed, a spokesperson informed us that since 2015 Cigna has limited the amount of urine testing it’ll cover.
That was around that time that Cigna sued a urine drug lab, called Sky Labs, in federal court, accusing it of insurance fraud.
“Put simply, the charges that Sky Labs submits to Cigna are inflated and fraudulent because they misrepresent the true amount billed to patients,” stated Cigna’s legal complaint filed in U.S. District Court of Southern Florida.
Cigna further accused Sky Labs of providing kickbacks to doctors who referred patients to their labs for drug tests. Cigna said that Sky Labs made “approximately $20 million in overpayments from Cigna.”
The lawsuit was settled out of court in 2016.
INTERACTIVE: Colorado Medicaid spending on urine drug tests
The U.S. Justice Department also brought a lawsuit alleging illegal kickbacks and false claims against Millennium Health, another major toxicology lab in the country. In that case, Millennium Health agreed to pay the federal government $256 million total in 2015. The payment was meant to resolve the allegations that the lab overbilled federal health care programs for “excessive and unnecessary urine drug testing” and for providing kickbacks to doctors.
Today, Cigna says it will not cover more than eight of the expanded round of tests per day.
Colorado’s Medicaid program, on the other hand, currently has no limits.
And that, as we discovered, is not without its consequences.
Our investigation found the state’s Medicaid program is now spending 26 times more per month for urine screens than it did in 2014.
Last year, that meant Colorado’s Medicaid program paid more than $16 million for urine screens, according to our analysis of data from the Colorado Department of Health Care Policy and Financing (HCPF).


As we found, it’s not more patients driving the bulk of the increase. It’s not the cost of each test either. What’s really behind the $16 million cost to Medicaid is the frequency of the testing done on individual patients.
In 2014, for example, Medicaid patients would get an average of 1.4 tests per month.
In 2016, the number shot up to 7.8 tests per month.
The reimbursement rate barely budged during that time.
Attorney Harry Nelson is critical of the amount of money pouring into labs across the state. “Basically, a lot of money is being spent to test for something where we already know the answer,” he told us.
We asked Dr. Judy Zerzan, Chief Medical Officer of HCPF, to respond to our findings that Colorado’s Medicaid program is now spending 26 times more per month on urine screens than it did in 2014.
“I think that’s a lot,” she replied.
She then told us it was something HCPF had simply missed.
“We had looked into this a couple of years ago when other states were having this problem, but we hadn’t refreshed it until you brought it to our attention,” she said.
One member of the Colorado legislature certainly wants to know more about what we found.
“I think this is something that’s deeply concerning to me right now,” said Rep. Joann Ginal.
She then promised to look into the matter further. We’ll let you know if it leads to any changes.


